You’re sitting on the couch, maybe scrolling through your phone, when you feel it. That little thumping in your neck or wrist. You check your smartwatch. It says 72. Or maybe 85. Suddenly, you’re wondering: what is your pulse rate should be anyway?
It’s a weirdly stressful question. We’ve been told since middle school gym class that 60 to 100 beats per minute is "normal," but that’s a massive range. It’s like saying a normal height for an adult is anywhere between five feet and seven feet. Technically true, but not exactly helpful when you're trying to figure out if your heart is doing what it’s supposed to do.
The truth is, your pulse is a moving target. It’s a liquid metric. It changes based on the coffee you drank twenty minutes ago, how well you slept, and even whether you’re slightly dehydrated.
The Baseline: What Science Says About the 60-100 Range
The American Heart Association (AHA) sticks to that 60-100 beats per minute (BPM) window for resting heart rate. But honestly, many cardiologists today argue that the upper end of that "normal" range is actually a bit high.
If you’re consistently sitting at 95 BPM while watching Netflix, your heart is working significantly harder than someone at 65 BPM. Over a decade, those extra beats add up. Some studies, like those published in the Journal of the American Medical Association, suggest that a resting heart rate consistently above 80 BPM might correlate with a higher risk of cardiovascular issues down the road.
Wait.
Don't panic.
If you just saw a 90 on your watch, it doesn't mean you're in trouble. It just means we need to look at the context. Are you stressed? Did you just walk up the stairs? Context is everything in cardiology.
When Lower is Actually Better
Athletes are the outliers here. You’ve probably heard stories about elite marathoners or Tour de France cyclists having resting pulses in the 30s or 40s. Miguel Induráin, a legendary cyclist, famously had a resting heart rate of 28 BPM.
For the average person, a pulse in the 50s is usually a sign of great cardiovascular efficiency. It means your heart muscle is strong enough to pump a high volume of blood with a single contraction. It doesn't have to twitch rapidly to keep your brain oxygenated. However, there is a condition called bradycardia. If your heart rate is below 60 and you feel dizzy, faint, or unusually tired, that’s when the low number becomes a medical conversation rather than a fitness badge of honor.
Why Your Number Is Jumping Around
Your heart is essentially a reactive sensor. It responds to your internal chemistry.
- Dehydration: When you’re low on fluids, your blood volume drops. Your heart has to beat faster to maintain blood pressure.
- Temperature: If it’s hot, your heart pumps more blood to your skin to help you cool down.
- Emotions: Anxiety triggers adrenaline. Adrenaline is a literal "go" signal for your sinoatrial node—the heart's natural pacemaker.
- Medications: Beta-blockers will drag that number down, while certain asthma inhalers or ADHD medications can send it spiking.
Think of your pulse like a tachometer in a car. You aren't always idling. Sometimes you’re revving. The goal is to make sure your "idle" isn't redlining for no reason.
Monitoring Your Pulse Rate: The Right Way to Do It
Most people check their pulse when they are already worried about it. This is a mistake. If you're anxious about your heart rate, the act of checking it will probably make it go up.
To get an accurate reading of what your pulse rate should be at rest, you need to do it first thing in the morning. Before you get out of bed. Before you check your emails or have a sip of espresso.
Put two fingers on your wrist—the radial artery—just below the base of your thumb. Don't use your thumb to feel, because your thumb has its own pulse and it’ll confuse the count. Count the beats for 30 seconds and multiply by two. Or, if you’re lazy like me, use a wearable, but make sure it's snug against your skin. Most optical sensors on watches fail if they're sliding around or if you have dark tattoos on your wrist.
Age, Gender, and the Pulse Gap
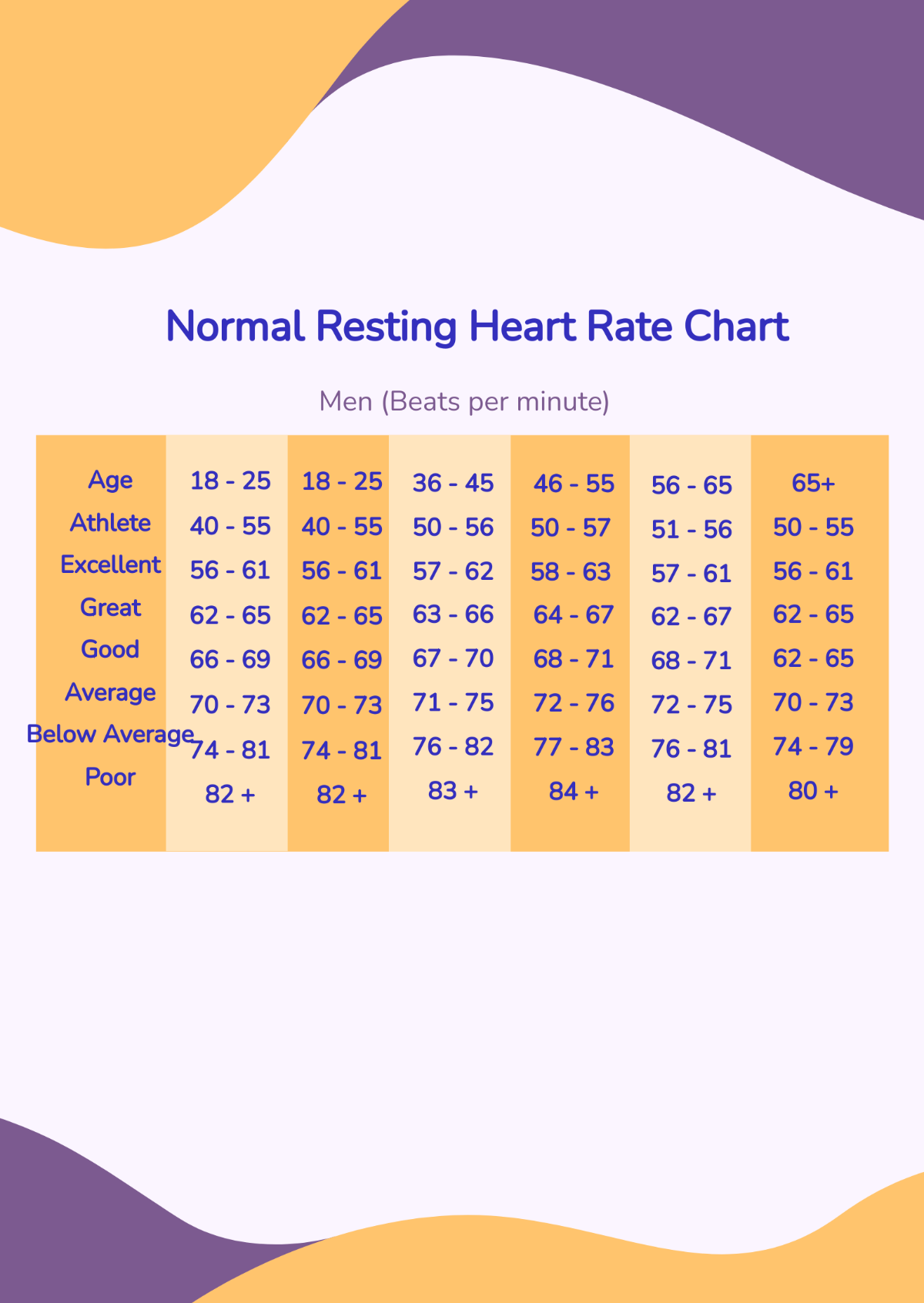
As we get older, our maximum heart rate tends to decrease, but our resting heart rate stays relatively stable unless our fitness levels change. Interestingly, women tend to have slightly higher resting heart rates than men—usually by about 2 to 7 beats per minute. This isn't a flaw; it's mostly due to the fact that women generally have smaller hearts that need to beat slightly more often to move the same amount of blood.
The Max Heart Rate Myth
You’ve probably seen the formula $220 - \text{age} = \text{Max HR}$.
Forget it.
It’s an old-school estimation that is frequently wrong. A 40-year-old might have a max heart rate of 195, or it might be 165. While it’s a decent starting point for zone training, it’s not a hard medical rule. If you’re trying to find your peak, a stress test with a professional is the only way to get a real number.
When Should You Actually Worry?
Numbers are just data points. Symptoms are what matter.
If your pulse is "high" but you feel fine, it might just be your baseline or a temporary spike. But if a high pulse is accompanied by chest pain, shortness of breath, or a feeling that your heart is "skipping" or "flopping" (palpitations), that’s a signal.
Tachycardia is the medical term for a resting heart rate over 100. If you’re sitting still and your heart is racing like you’re on a treadmill, that’s an issue. It could be an electrical glitch in the heart like Atrial Fibrillation (Afib), or it could be something as simple as a thyroid imbalance.
Practical Steps to Lower a High Resting Heart Rate
If you’ve discovered your resting rate is higher than you’d like, you aren't stuck there. The heart is a muscle. You can train it.
- Interval Training: You don't need to run for hours. Short bursts of high intensity followed by recovery periods teach your heart how to bounce back to a lower rate quickly.
- Magnesium and Potassium: These electrolytes are vital for the electrical signals in your heart. If you're deficient, your rhythm can get twitchy.
- Vagal Tone: Your Vagus nerve is the "brake" for your heart. Deep, diaphragmatic breathing—the kind where your belly expands—activates the parasympathetic nervous system and can drop your pulse by 5-10 beats in minutes.
- Sleep Hygiene: Chronic sleep deprivation keeps your cortisol levels high. High cortisol equals a high pulse.
Next Steps for Your Heart Health
Start by tracking your resting heart rate for seven days straight, every morning when you wake up. Take the average of those seven days. This is your true baseline. If that average is consistently above 85 or 90, schedule a basic check-up to rule out things like anemia or thyroid issues.
Keep a log of what you were doing when you noticed a spike. Was it after a big meal? After a fight with a spouse? Having this data ready for a doctor makes you an active participant in your health rather than just a worried observer.
If you use a wearable, look at your "Heart Rate Recovery" (HRR) after exercise. See how much your pulse drops in the first two minutes after you stop moving. A drop of 12 beats or more in the first minute is generally a sign of a healthy, responsive heart.
/i.s3.glbimg.com/v1/AUTH_08fbf48bc0524877943fe86e43087e7a/internal_photos/bs/2025/H/e/ewwgKCQCSopdUJUwy6DA/imagem-2025-04-27-114802986.png)

