If you’ve ever felt like someone is jamming a hot needle into the side of your head, you’re probably dealing with an ear drum with ear infection combo that is, frankly, miserable. It's one of those pains that makes it impossible to focus on anything else. You can't sleep. You can't think. Even chewing a piece of toast feels like a structural threat to your skull.
Most people think the pain is just "the infection." But honestly? The pain is mostly about pressure.
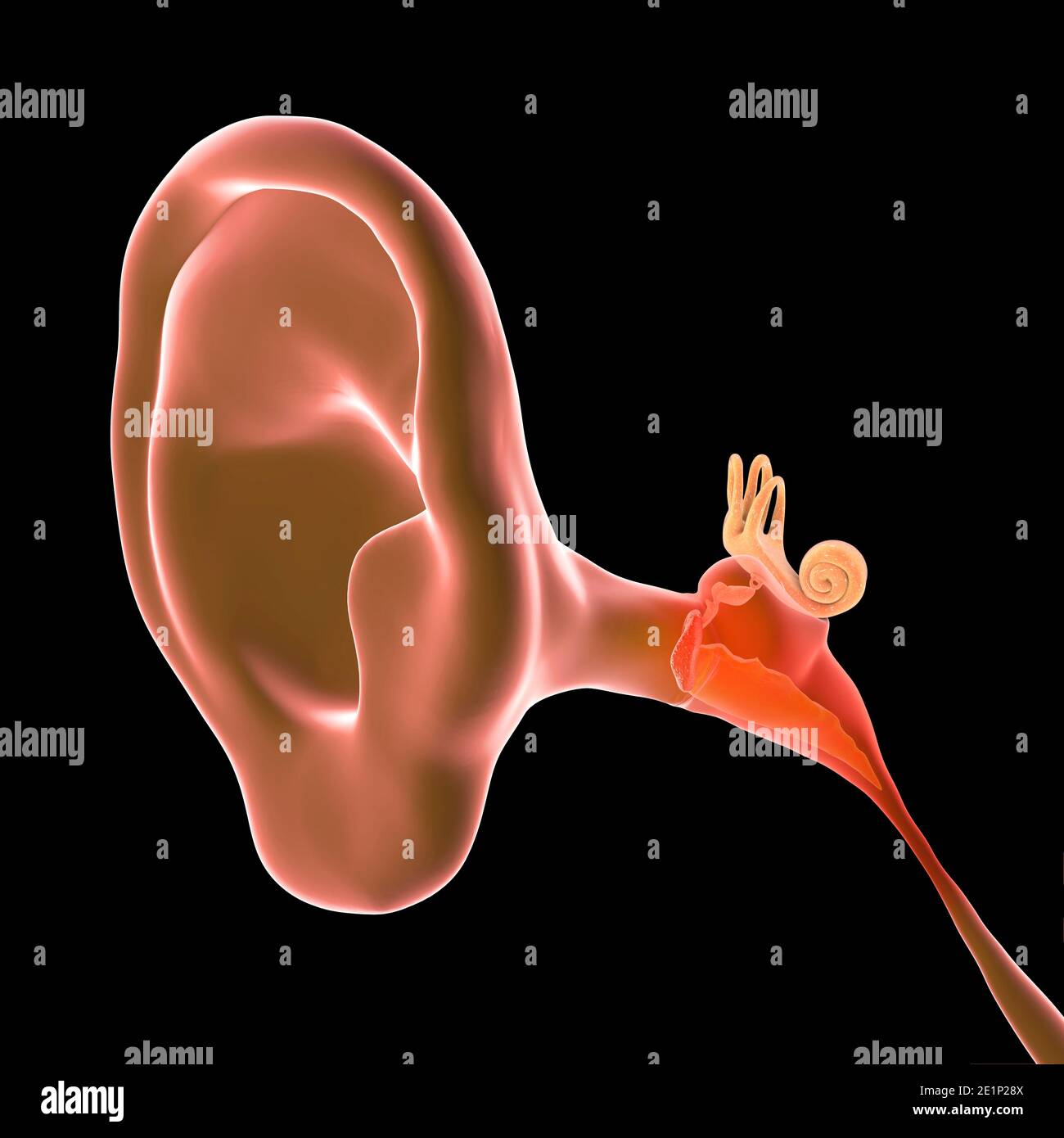
Think of your eardrum—the tympanic membrane—as a tiny, taut drum skin. It’s incredibly thin. Behind that skin is the middle ear, a space that is supposed to be filled with air. When you get a cold or allergies, the Eustachian tube (the drainage pipe for your ear) swells shut. Fluid gets trapped. Bacteria move in. Suddenly, that air-filled space becomes a pressurized swamp. Your eardrum is being pushed outward by pus and fluid, stretching those sensitive nerves to their absolute limit. That’s why it hurts so much.
What's Actually Happening to Your Eardrum?
It’s not just "sore."
When you have an ear drum with ear infection, the membrane physically changes. If a doctor looks at it with an otoscope, they aren't just looking for redness. They’re looking for "bulging." A healthy eardrum is translucent and pearly gray. An infected one looks angry, red, and opaque. Sometimes it even looks yellow because of the purulent fluid (pus) sitting right behind it.
Dr. Eric Voigt, a renowned otolaryngologist at NYU Langone, often points out that the "light reflex"—the way a doctor's light bounces off a healthy eardrum—disappears when there’s an infection. The drum becomes distorted.
Sometimes, the pressure gets so high that the eardrum actually tears. This is a perforated eardrum. It sounds terrifying, and it's definitely not ideal, but oddly enough, the moment it pops, the pain usually vanishes. Why? Because the pressure is finally gone. You’ll see fluid draining out of the ear canal, which is gross, but it's your body's way of hitting a pressure-release valve.
The Fluid Factor: It's Not Always Bacteria
There is a huge difference between a "hot" infection (Acute Otitis Media) and just having fluid back there (Otitis Media with Effusion).
One involves screaming pain and fever. The other feels like you're underwater.
If you have an ear drum with ear infection symptoms but no fever and it’s just muffled, it might be "glue ear." This happens when the fluid is thick and sticky but not necessarily teeming with bacteria. Doctors are often hesitant to prescribe antibiotics for this because, well, they won't do anything for a viral clog. We’ve become a bit too reliant on the "pink stuff" (Amoxicillin), but the American Academy of Pediatrics has been pushing a "watchful waiting" approach for decades now to prevent antibiotic resistance.
Why Adults Get This Too
We tend to think of this as a "kid problem." It’s true, kids have shorter, more horizontal Eustachian tubes. Gravity doesn't help them drain. But adults get hammered by this too, usually following a nasty bout of the flu or a chronic sinus issue. If you’re an adult with a recurring ear drum with ear infection, it might not even be your ear's fault. It could be your jaw (TMJ) or even a structural issue in your nose like a deviated septum.
The Risks of Ignoring the Pressure
You shouldn't panic, but you shouldn't ignore it either.
If the infection stays trapped for too long, it can start to erode the tiny bones in your ear—the malleus, incus, and stapes. These are the smallest bones in your body. They vibrate to help you hear. If they get damaged, you’re looking at permanent hearing loss.
In rare cases, the infection can spread to the mastoid bone behind your ear. This is called mastoiditis. It used to be a leading cause of death in children before antibiotics. Now, it’s rare, but if you see redness or swelling on the bone behind your ear, that’s an ER visit. No questions asked.
Home Care vs. Doctor Visits
Don't put things in your ear. Please.
No Q-tips. No "ear candles" (which are basically a scam and incredibly dangerous). No hydrogen peroxide unless a doctor told you to.
If you're managing an ear drum with ear infection at home while waiting for an appointment, heat is your best friend. A warm (not boiling) compress against the ear can help soothe the throbbing. Over-the-counter pain relievers like ibuprofen are actually more effective than most "ear drops" because they tackle the inflammation from the inside out.
- Keep your head elevated. Sleeping propped up on two pillows helps the fluid drain downward rather than pooling against the drum.
- Decongestants. If your nose is clogged, your ears stay clogged. Using a nasal steroid spray like Flonase can sometimes help open the Eustachian tube entrance, though it takes a few days to work.
- Avoid flying. If you have a pressurized ear and you get on a plane, the change in cabin pressure can literally rupture your eardrum. It’s an agonizing experience.
When Do You Need Tubes?
For people who get an ear drum with ear infection every time they catch a sniffle, "tubes" (myringotomy tubes) are the gold standard. They are tiny cylinders inserted into the eardrum to create a permanent air vent. It’s a 15-minute surgery. They eventually fall out on their own. They don't "cure" the infection, but they prevent the pressure from ever building up, which keeps the pain away and saves your hearing.
Real Steps for Relief
If you feel that tell-tale fullness starting, act fast.
First, start a saline rinse (like a Neti pot) to keep your sinuses clear. Use distilled water only—never tap water. Second, stay hydrated. It keeps the mucus in your ear from turning into that "glue" that is so hard to clear. If you start to see a "pumping" sensation in your hearing—where you can hear your heartbeat in your ear—it's a sign of significant inflammation.
Check your temperature. If a high fever kicks in alongside the ear pain, that’s usually the sign that the bacteria have taken over and you need a prescription. If you're just feeling "stuffy," try the Valsalva maneuver: pinch your nose, close your mouth, and very gently try to blow air out of your nose. If you hear a "pop," your Eustachian tube just opened. If it hurts, stop immediately. You don't want to force bacteria deeper into the middle ear.
Monitor the pain levels for 48 hours. Many viral ear infections resolve on their own without meds. But if the pain is worsening or you notice any facial weakness or severe dizziness, get to a clinic. Protecting the delicate mechanics of your eardrum is worth the co-pay.

/i.s3.glbimg.com/v1/AUTH_08fbf48bc0524877943fe86e43087e7a/internal_photos/bs/2025/H/e/ewwgKCQCSopdUJUwy6DA/imagem-2025-04-27-114802986.png)
